|
Intracorneal rings for the correction of pellucid marginal degeneration. Rodriguez-Prats J, Galal A, Garcia-Lledo M, De La Hoz F, Alió JL. One or two INTACS segments for the correction of keratoconus. J Cataract Refract Surg 2006 32:756–761.Īlió AJ, Artola A, Hassanein A, Haroun H, Galal A. Analysis of results related to good and bad outcome of INTACS implantation for correction of Keratoconus. Invest Ophthalmol Vis Sci 1995 36 suppl:308.Īlió JL, Shabayek MH, Belda JI, Correas P, Feijoo ED. Numerical simulation of topographical alterations in the cornea after intrastromal corneal ring (ICR) placement. Model for deriving the optical performance of the myopic eye corrected with an intracorneal ring. Intrastromal corneal ring-12months sighted myopic eyes. Intrastromal corneal ring-one year results of first implant in humans: a preliminary non-functional eye study. Flattening of the curvature with intrastromal corneal rings of increasing thickness-an eye bank eye study. J Refractive Surg 1987 3:227–232.īurris TE, Baker PC, Ayer et al. The intrastromal corneal ring-two cases in rabbits. J Refract Surg 2004 20:162–165.įleming JR, Reynolds AI, Kilmer L. Lamellar crescentic resection for pellucid marginal corneal degeneration. Javadi MA, Karimian F, Hosseinzadeh A, Noroozizadeh HM, Sa’eedifar MR, Rabie HM. Compressive C-shaped lamellar keratoplasty: a surgical alternative for the management of severe astigmatism from peripheral corneal degeneration. Topographic analysis in pellucid marginal corneal degeneration and keratoglobus. Keratectasia in 2 cases with pellucid marginal corneal degeneration after laser in situ keratomileusis. Japan J Ophthalmol 2003 47:523–525.įogla R, Rao SK, Padmanabhan P. Progression of pellucid marginal degeneration and higher-order wavefront aberration of the cornea. Kamiya K, Hirohara Y, Mihashi T, Hiraoka T, Kaji Y, Oshika T. The results of penetrating keratoplasty for pellucid marginal corneal degeneration. Keratoconus with pellucid marginal corneal degeneration. Kayazawa F, Nishimura K, Kodama Y, et al. Corneal topography of pellucid marginal degeneration. 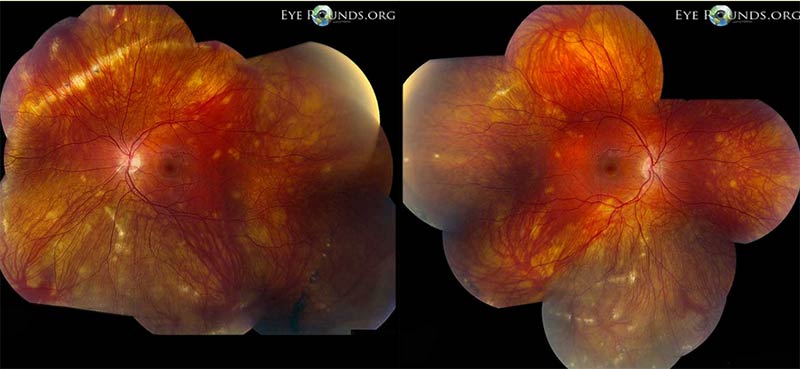
Maguire LJ, Klyce SD, McDonald MB, Kaufman HE. Sridhar MS, Mahesh S, Bansal AK, Nutheti R, Rao GN. Corneal topography in atypical pellucid marginal degeneration. Superior pellucid marginal corneal degeneration with hydrops. This process is experimental and the keywords may be updated as the learning algorithm improves. 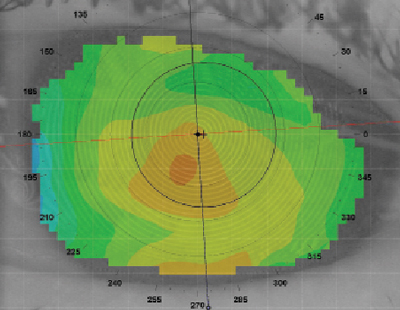
These keywords were added by machine and not by the authors. Usually, present with reduced visual acuity owing to high irregular astigmatism in the fourth to fifth decades of life ( 4). The area between the limbus and thinning is clear, without scarring, lipid deposition, or vascularization. Typically the thinning extends from the 4-o’clock position to the 8-o’clock position, 1 mm from the limbus with intact epithelium and normal corneal thickness superiorly. The degeneration is distinguished from other ectatic corneal disorders by its characteristic location and the absence of inflammatory signs. 
Although classically described as an inferor entity, the site of involvement can be in any quadrant of the cornea, including the superior part, which is termed superior PMCD ( 2, 3). It is a bilateral disease, although one eye may be affected earlier and clinically diagnosed, while the other eye has no clinical features ( 1). Pellucid marginal corneal degeneration (PMCD) is a noninflammatory ectatic corneal disorder mostly involving the inferior half of the cornea in a crescentic fashion (Fig.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
